At a Glance
CPAP therapy may help improve breathing and sleep quality in people with both asthma and obstructive sleep apnea, but it isn’t a direct treatment for asthma. Asthma and sleep apnea are closely linked and can worsen each other, making it important to address both conditions together. If symptoms worsen or CPAP is difficult to tolerate, a healthcare provider can help adjust your treatment plan.
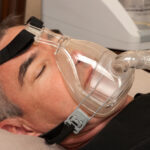
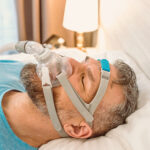
For people with both asthma and sleep apnea, CPAP therapy can help stabilize nighttime breathing and reduce sleep disruption. By keeping the airway open during sleep, it may also lessen nighttime asthma symptoms like coughing, wheezing, and shortness of breath.
However, CPAP isn’t a direct treatment for asthma, and some users may experience irritation or dryness if their settings aren’t optimized. In this article, we’ll explore how CPAP affects asthma, its potential benefits and drawbacks, and tips for using it more comfortably.
Make CPAP Cleaning Quick and Easy
Shop CPAP cleaning supplies like wipes, brushes, and soap from Sleep Doctor to keep your therapy hygienic and effective.

How Are Asthma and Sleep Apnea Connected?
Obstructive sleep apnea (OSA) and asthma are common breathing disorders that affect up to 30% and 8% of adults in the U.S., respectively. And there’s often an overlap between the two conditions. In fact, people with asthma may be at more risk for sleep apnea than the general public. One study completed across four years found that 27% of people with asthma also had OSA, while only 16% of people without asthma developed OSA.
While there’s a clear link between the two, researchers are still looking into why. Some hypothesize the connection may be due to asthma’s effects on the body’s parasympathetic tone, or the level of activity of the parasympathetic (“rest and digest”) nervous system.
Anatomy may also play a part. People with asthma may have nasal obstruction due to allergic rhinitis, narrow airways including adenoid or tonsil enlargement, or increased potential for upper airway collapse, which can all make OSA symptoms more severe.
Asthma may also negatively impact the neural receptors in the upper airway that control the muscles within your breathing passages. OSA can make asthma worse, as it can irritate and inflame your airways enough to affect your anatomy.
Does CPAP Help Asthma?
CPAP therapy can help improve asthma symptoms, especially for those with both asthma and sleep apnea. Researchers say that CPAP is a worthwhile treatment for some people with asthma, and that it may be particularly helpful for people with obesity, because CPAP can counteract breathing problems that come as a result of increased pressure on their airways.
The pressurized air can decrease wheezing and coughing while supporting breathing passages. The person is also getting overnight delivery of filtered and humidified air, reducing exposure to allergens in the sleep environment.
CPAP can reduce nighttime asthma attacks, especially in the early morning hours, and help improve sleep quality. A review of existing studies shows that CPAP therapy can improve quality of life for people with both OSA and asthma. CPAP appears to be especially helpful for decreasing asthma severity in people with severe OSA and asthma that’s poorly controlled.
Can CPAP Make Asthma Worse?
Some people find CPAPs uncomfortable, especially when first beginning therapy. Compliance is important, though, and stopping therapy for even a short amount of time can worsen OSA symptoms.
Researchers aren’t sure exactly how long you should use your CPAP to reduce asthma symptoms, but in general, four hours is the minimum, with the ultimate goal being to use it as much as possible during sleep.
One of the most common CPAP complaints is dry air, which can irritate breathing passages and potentially make asthma worse. Cold air can be uncomfortable too, but heated CPAP humidifiers can target both issues. Warm, humid air moistens the nasal passage and throat and makes the pressurized air more comfortable to breathe. Many modern CPAP machines have climate features that let you make adjustments to humidity levels and air temperature.
A poorly fitting mask can also cause problems. When masks don’t seal correctly, air can leak from the sides of the mask and create dryness and breathing discomfort. If you suspect that your mask doesn’t fit correctly, you can try a different style or cushion size. Also, keep in mind that people who breathe through their noses may need a different mask style than those who breathe through their mouths. If you can’t find a mask with minimal leak issues, check in with your provider.
Tips for Using CPAP With Asthma
- Use a humidifier: Heated humidification and a heated hose can make a significant difference in comfort for everyone who uses a CPAP, but especially those with asthma.
- Keep equipment clean: Bacteria, germs, and irritants may build up inside your CPAP machine and accessories. Clean your CPAP equipment according to manufacturer specifications using warm water and mild soap. Avoid using ozone or ultraviolet (UV) light CPAP cleaners.
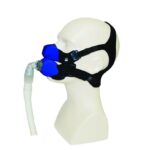
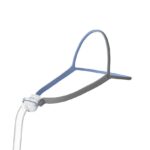
- Use the correct mask: The wrong mask for your face size or breathing habits can cause leaks. Make sure to get a nasal mask, nasal pillow, or full-face mask with the right size cushion for your face and don’t be afraid to try multiple styles to get the best fit.
- Adjust ramp settings: CPAP machines with a ramp feature can be easier for people who don’t tolerate pressure well. Ramp settings start therapy at a low pressure that slowly ramps up to full pressure by the time you fall asleep.
When to Talk to Your Doctor
If you notice increased coughing or wheezing with CPAP use, talk to your doctor. Likewise, if your breathing feels worse during or after CPAP therapy, you should consult your provider.
Pressure settings are prescribed and shouldn’t be changed by anyone but your doctor. If you’re having trouble tolerating air pressure, try your machine’s ramp feature or expiratory pressure relief (EPR). You can also ask your doctor about lowering your settings or trying an automatic positive airway pressure (APAP) or bilevel machine.
If you suspect you have sleep apnea but haven't been diagnosed, the first step is a sleep study, which your doctor can prescribe after evaluating your symptoms and medical history. You can get an in-person sleep study done at a sleep center or you can take an at-home sleep test easily from your own bedroom if your doctor thinks that’s an option.
Medical Disclaimer: This content is for informational purposes and does not constitute medical advice. Please consult a health care provider prior to starting a new treatment or making changes to your treatment plan.