At a Glance
A survey found that many adults are unfamiliar with sleep apnea, and 78.4% of people who think they understand the condition cannot correctly define it. This gap in awareness may delay diagnosis and treatment, even though many people report symptoms such as snoring, fatigue, or trouble concentrating that could signal sleep apnea.
Chaundra Scott had no idea what sleep apnea was until she was diagnosed with it in 2018. Scott, 41, of Maryland, only knew that she snored heavily and would always wake up feeling exhausted. Sometimes she’d even nod off during the day.
“My doctors couldn’t pinpoint anything,” Scott says. When a physician suggested Scott take a sleep study for severe sinus issues, she finally learned what was causing her fatigue.
Scott's sleep apnea awareness is similar to that of 30.7% U.S. adults who say they don’t know what sleep apnea is, according to a SleepApnea.org survey of 1,250 people ages 18 and older. But that number might be higher: 78.4% of respondents who think they know what sleep apnea is were incorrect, misidentifying its definition or confusing it with everything from teeth-grinding and insomnia to cardiac arrest.
Although just 4.8% of adults have been diagnosed with obstructive sleep apnea (OSA), with 3.8% diagnosed with central sleep apnea (CSA), according to the survey, research puts the OSA population at as high as 37.3% of adults1. That's quite a few people who may have a sleep disorder they aren't even familiar with, to say nothing of how it's treated.
“People out there have no idea what sleep apnea is and no idea that they're having trouble breathing in their sleep,” says Dr. Joseph Krainin, SleepApnea.org's medical advisor. “Frankly, they have no idea that the symptoms they might be having, like waking up feeling tired or having high blood pressure, could be linked to a sleep problem.”
Think You Might Have Sleep Apnea? Get Answers at Home
Sleep Doctor’s home sleep study makes diagnosis simple — no lab visit required. Get results reviewed by a sleep specialist and guidance on what to do next.

Survey Results
- 30.7% of surveyed U.S. adults say they don't know what sleep apnea is.
- 78.4% of adults who say they know what sleep apnea is actually don't.
- 5.3% of adults have been diagnosed with sleep apnea.
- 17.8% of adults suspect they may have sleep apnea.
- 40.3% of adults diagnosed with sleep apnea have not tried or been prescribed any treatment.
- 61.8% of adults say they know what a CPAP machine is, but 57.6% of them don't know what CPAP stands for.
Making Sense of the Sleep Apnea Education Gap
Understanding sleep apnea and its signs, including snoring, is central to an accurate and timely diagnosis. The health risks of untreated sleep apnea are significant. It starts with knowing what sleep apnea is in the first place.
A bit more than half of adults in the survey, or 52.1%, can identify sleep apnea by its general definition: a sleep disorder that causes frequent pauses in breathing while you sleep. But only 21.4% correctly identified it by more technical terms: a constriction or blockage of the airway during sleep (OSA) or a communication disruption between the brain and throat muscles (CSA).
About the same amount (19.8%) confused it with the definition of insomnia, and 17.1% defined it as full-on heart stoppages that occur at least three times an hour.
When Charlene Jaszewski's dad received a diagnosis of sleep apnea years ago, she thought the term referred to “just when you wake up gasping for air.” “And that doesn't happen to me,” she says. “I also thought it had to do with how easily you went to sleep.”
So when the 54-year-old from Minneapolis received her own severe sleep apnea diagnosis “completely by accident” in July 2022 after undergoing a sleep study for bariatric surgery, she wasn’t expecting it.
Getting Ahead of Sleep Apnea's Symptoms
That's a reasonably common way in which people are introduced to sleep apnea, Dr. Krainin says. In some ways, the symptoms are hiding in plain sight.
“By definition, you're asleep. So you're unaware of what's happening,” he says. “And even when people are confronted with videos of themselves snoring loudly, stopping breathing, or making gasping noises, it's hard for them to believe.”
Although 5.3% of adults in the survey received a sleep apnea diagnosis of some kind, another 17.8% suspect they have sleep apnea. People who suspect they have sleep apnea are onto many of the classic symptoms, as they're 84% more likely than average to snore, 59.7% more likely to experience insomnia, and 54.3% more likely to have trouble focusing or concentrating.
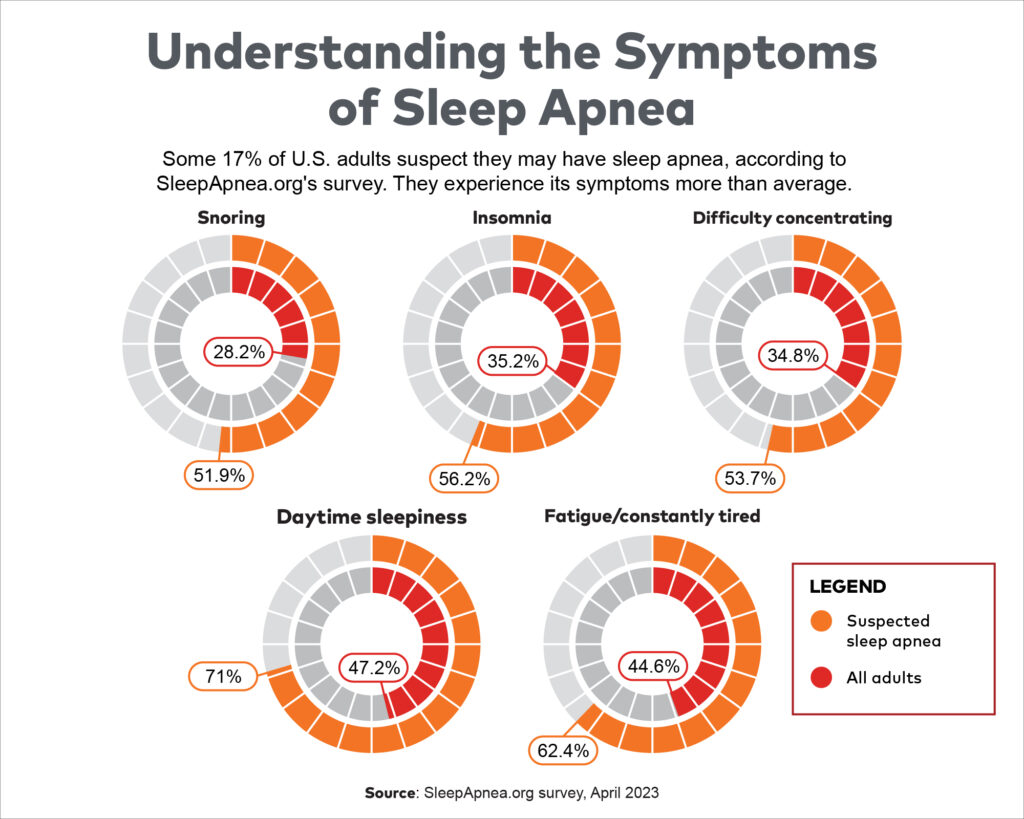
Some 71% of people who think they may have sleep apnea have daytime sleepiness, too. Acknowledging the symptoms as symptoms may be easier said than done, however.
“In my experience, it usually takes years for people to be willing to consider taking action,” Dr. Krainin says. “And the first step in that is a sleep study,” as well as speaking with a physician.
Taking Sleep Apnea Seriously
Mark Joseph of St. Louis received a sleep apnea diagnosis as a young adult. Now 32, he takes extra care and patience to teach his family and friends about it.
“I explain things that might be confusing and answer any questions they have so they can understand what I'm going through,” he says. “Talking with them has been a great way to gain support and spread awareness. They now know about my sleep apnea and how it affects me daily.”
Sleep apnea can raise your risk of having other health problems2. By and large, people who have heard of sleep apnea don't underestimate it, with 76.7% of adults agreeing that it has serious health implications, according to the survey. One in four adults considers sleep apnea “extremely serious.” Only 7.4% say sleep apnea is “nothing to worry about;” among respondents who selected the correct definition of sleep apnea in the survey, that drops to 3.9%
How Familiar Are We With Sleep Apnea Treatment?
Scott says her sleep apnea now comes up frequently during routine appointments and whenever she has outpatient surgery. Jaszewski has recognized its connection to fatty liver disease3, high blood pressure4, and high cholesterol — “like, all the things that I have.”
What happens after diagnosis? Sometimes, nothing. According to the survey, 40.3% of adults diagnosed with sleep apnea have not tried or been prescribed any treatment.
One of the better-known OSA treatments is continuous positive airway pressure (CPAP) therapy, via a CPAP machine. According to the survey, 61.8% of adults say they know what a CPAP machine is.
CPAP machines have come a long way since starting as a reverse paint compressor. The survey put respondents' knowledge to the test, asking them to select images of CPAPs versus other objects. Although 81.6% could identify a CPAP machine out of the lineup, only 9.5% correctly identified all of the CPAPs they were shown. And 0.7% selected only CPAPs and no other objects, including an old paint compressor.

More than half of adults (57.6%) who say they knew what a CPAP was did not know what the abbreviation stands for. Meanwhile, 29.8% of adults who've received a sleep apnea diagnosis use a CPAP or bilevel positive airway pressure (BiPAP) machine, both of which can be used for CSA and other breathing disorders. Aside from lifestyle changes (38.7%), it was the most popular treatment option among respondents.
The machines can come with a learning curve, however: Jaszewski says she needed time to adjust to its mask. The machines require a prescription, as well.
Dr. Kent Smith, a dental sleep medicine specialist and chief medical officer of the Sleep Dallas sleep clinic in Frisco, Texas, says he frequently has to explain the treatment options to his patients that have sleep apnea. He says that research shows that oral appliances, which 8.6% of survey respondents with sleep apnea use, can be effective for mild or moderate sleep apnea5.
Whatever the situation, education on what sleep apnea is and how to treat it is key, he says, as Dr. Krainin also notes.
“If you're getting enough sleep, at least seven to eight hours regularly, and you're still waking up feeling tired, then it's time to go talk to your doctor,” Dr. Krainin says.
Methodology
The survey commissioned by SleepApnea.org was conducted on the online survey platform Pollfish on April 5, 2023. Results are from 1,250 survey participants in the United States who were age 18 or older at the time of the survey. All respondents attested to answering the survey questions truthfully and accurately.








