At a Glance
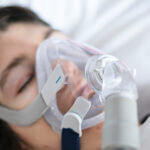
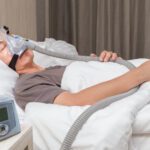
CPAP compliance refers to how consistently you use your CPAP machine, which is typically defined by the “4-hour rule”: using the device at least 4 hours per night on at least 70% of nights within a 30-day period. Meeting this threshold helps ensure your treatment is effective and may be required for insurance to continue covering your CPAP equipment and supplies.
Whether you’re just getting started using a CPAP machine or have been using one for a while, CPAP compliance is important to make sure you’re getting all the benefits from therapy. If you don’t use your CPAP as often as your doctor recommends, your symptoms may not improve or may return back to their original severity.
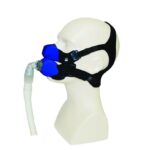
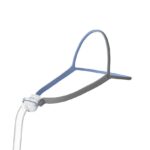
Some people who have difficulty tolerating CPAP therapy may feel more comfortable after making adjustments to their mask or to their machine settings. If you experience difficulties using a CPAP, talk with your doctor to find a solution that works for you.
Below, we’ll explain what CPAP compliance means, how it’s measured, why it matters, and tips to help you stay consistent with therapy.
What Is CPAP Compliance?
CPAP compliance is the number of hours per night and nights per week that an individual uses their CPAP machine. Some sleep experts also call it “CPAP adherence.” Most insurance companies in the United States consider people who use their CPAP machine for at least four hours per night and at least five nights per week to be compliant.
About half of all people who were prescribed CPAP machines use them for less than four hours per night. However, studies have found that people who used their CPAP for more hours had greater improvements in their sleep apnea symptoms and risk factors. For example, the best evidence for reducing cardiovascular risk was demonstrated with six or more hours per night.
How Is CPAP Compliance Measured?
CPAP compliance is measured by tracking how often and how long you use your CPAP machine each night. Most modern CPAP machines record usage data — the amount of time that they are on and that an individual wears the mask — which can be reviewed by your doctor or insurance provider.
However, some older machines only measure how long the machine is on. These older machines may overestimate CPAP compliance. For example, if a person takes off their mask but leaves the machine running, an older machine may record that time as CPAP compliance.
Never Run Out of CPAP Supplies and Save 15%
Shop CPAP supplies from Sleep Doctor and get masks, filters, and tubing at 15% off with Subscribe & Save.

Why CPAP Compliance Matters
CPAP compliance is important because when people with sleep apnea use their CPAP machine for more hours, they receive more improvements to their health and symptoms. Studies have found many benefits to CPAP compliance:
- Less daytime sleepiness
- Improved memory
- Higher quality of life
- Improved daily functioning
- Lower blood pressure
- Fewer motor vehicle accidents
Early CPAP compliance is important for long-term treatment success. People who routinely use their CPAP machine as recommended during their first three months of treatment are more likely to still be using their CPAP machine over the coming years.
However, this doesn't mean that you should give up if you weren't successful in your first three months. Talk to your doctor if you have any discomfort or side effects while using your CPAP machine.
People whose symptoms do improve while using a CPAP machine may notice that their symptoms return soon after they stop or reduce CPAP use. Research has found that reducing CPAP use is linked to an increased apnea-hypopnea index (AHI), which often translates to more daytime sleepiness and higher blood pressure and pulse rate.

How to Get a Compliance Report From a CPAP Machine
Most CPAP machines can create reports with information on CPAP compliance, effectiveness, and air leaks, as well as more detailed reports with additional information. These reports can be downloaded using Wi-Fi, modem, or a digital data card.
Many devices have a built-in screen or menu where you can view basic usage stats, such as hours used and nights worn. More detailed reports are often available through a mobile app or online patient portal connected to your device.
If you need a formal compliance report for insurance or your healthcare provider, your durable medical equipment (DME) supplier or doctor’s office can typically download and share it. Some machines also store data on an SD card that can be brought in for review.
Most doctors check over CPAP reports every few weeks to months while you get used to using a CPAP machine. Once you're using your CPAP machine regularly, your doctor will probably check your CPAP machine reports at least once a year, and any time you have new or different symptoms related to sleep apnea.
Since many newer devices are accessible remotely, this means it’s possible for you to contact your doctor's office with a specific complaint (e.g., the pressure feels too high). The doctor can log into the machine, look at the detailed data, and make a change to your device — all without you having to bring the device to the office.
How to Read a CPAP Compliance Report
The CPAP compliance report will show a graph, table, or both showing the number of days and hours you used the CPAP machine over a particular period of time. The report may contain additional information, such as the average number of hours the CPAP machine was used per night or the percentage of nights during which it was used for four or more hours.
You may also see usage trends over time, including how many nights you used the machine and your average nightly use. Some reports include additional data, such as mask leak rates or AHI, which can help your provider assess how well your therapy is working.
If the report shows that you're using the CPAP machine less than four hours per night for at least 70% of nights, then your doctor may recommend changes to improve your compliance. However, your doctor may recommend you increase your CPAP use even if you meet these targets, particularly if your symptoms don’t improve after starting CPAP therapy.

How to Get Used to CPAP Therapy
It’s okay if you aren’t able to wear your CPAP machine all night on your first night using it. Most people adjust to CPAP therapy within their first two weeks to three months. However, it’s important to talk to your doctor as soon as possible if you have any difficulties with CPAP therapy. Your doctor can help you troubleshoot CPAP problems, such as:
- Adjusting the pressure if it’s uncomfortable
- Refitting or changing the mask if it's painful or causes dry eye or claustrophobia
- Warming and humidifying the air if it irritates your nose
- Adding a chin strap if you have air leaks
- Allergy testing or decongestant nasal spray if you have a stuffy nose
In addition, your doctor may also recommend you attend one or two group sessions with other people who use CPAP therapy and get check-in phone calls. These sessions and calls can help you to feel more confident and better meet your goals.
Experts recommend tips that people who use CPAP machines can try at home to improve their CPAP compliance:
- Ask your bed partner or roommate, if any, to support and encourage your CPAP therapy.
- Adjust mask straps if they feel too tight or too loose.
- Use your CPAP for brief periods during the day to help you get used to it.
- Slowly increase the length of time you use your CPAP until you meet your goals.