At a Glance
A CPAP machine treats sleep apnea by delivering a steady stream of pressurized air through a mask and tubing system to keep the airway open during sleep. The machine draws in and filters room air, then sends it through the hose to the mask, preventing airway collapse, reducing snoring and breathing interruptions, and helping maintain stable oxygen levels overnight.
A continuous positive airway pressure (CPAP) machine is a device that pumps a steady stream of pressurized air into your airway while you sleep. It's the most common and typically the first recommended treatment for people with sleep apnea, a sleep disorder that affects breathing at night.
CPAP has been shown to improve sleep and to reduce the risk of health issues that untreated sleep apnea can cause. Learning about what a CPAP machine is and how it compares to other sleep apnea treatments can help you make informed decisions about managing your sleep apnea.
Overwhelmed by Your Options? We Make CPAP Simple
Sleep Doctor helps you find the right machine, masks, and supplies, so you can start therapy with confidence from day one.

What Does CPAP Stand For?
CPAP stands for continuous positive airway pressure and is one of several forms of positive airway pressure (PAP) therapy, which all work by delivering air through a mask but differ in how the pressure is controlled:
- APAP (automatic positive airway pressure): automatically adjusts the air pressure throughout the night based on your breathing patterns
- BiPAP or BPAP (bilevel positive airway pressure): provides two pressure levels: one for inhalation and a lower one for exhalation
- EPAP (expiratory positive airway pressure (EPAP): nasal valves that use your own exhaled breath to generate pressure and keep the airway open
How Does a CPAP Machine Work?
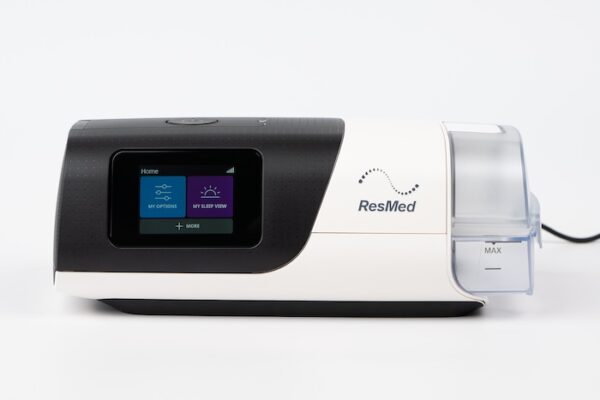
A CPAP machine works by delivering a steady stream of pressurized air through a hose and mask to keep your upper airway open while you sleep. This gentle airflow acts like a pneumatic splint, preventing the soft tissues in the throat from collapsing and blocking the airway—a common cause of obstructive sleep apnea.
The machine draws in room air, filters it, and pressurizes it to a level prescribed by your doctor based on your sleep study results. That pressurized air flows into your mask to maintain continuous airway support throughout the night. Many CPAP machines also include optional comfort features—such as heated humidifiers, ramp settings, and exhalation relief—to make breathing feel more natural and reduce dryness or irritation.
By preventing breathing pauses, CPAP helps restore normal oxygen levels, reduce snoring, and promote deeper, more restorative sleep.
What Is a CPAP Machine Used For?
CPAP therapy is used to treat the two main types of sleep apnea: obstructive sleep apnea (OSA) and central sleep apnea (CSA). Both types of sleep apnea cause breathing interruptions during sleep, and CPAP therapy reduces the number of breathing interruptions and snoring severity.
In addition, a CPAP machine is also sometimes used to treat:
- Chronic obstructive pulmonary disease (COPD)–related breathing problems during sleep
- Obesity hypoventilation syndrome (OHS)
- Heart failure–related breathing disturbances
- Certain neuromuscular disorders that affect nighttime breathing
How Do You Use a CPAP Machine?
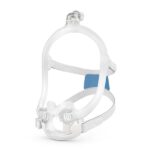
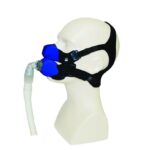
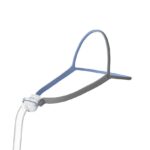
To operate a CPAP machine, you wear a mask that fits snugly over your nose and/or mouth. The mask connects to the CPAP machine through a narrow hose. When you turn on the machine, it gently directs filtered, pressurized air into the mask. There are three main types of masks:
- Full-face mask: A full-face (oronasal) mask covers both the nose and mouth.
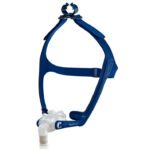
- Nasal mask: A nasal mask covers the nose and extends from the bridge of the nose to the upper lip.
- Nasal pillow: A nasal pillow includes two tubes inserted into the nostrils.
Your doctor can help you with how to choose a CPAP mask and also help customize the air pressure. Your doctor usually determines the air pressure based on the results of a sleep study in a clinic. If you find your set pressure level to be uncomfortable, your doctor can reprogram your machine, or you can try a new mask.
How Do You Clean a CPAP Machine?
Regularly cleaning your CPAP machine keeps it working properly and reduces your risk of irritation, infection, or exposure to mold and bacteria. Most cleaning can be done at home with mild soap and warm water, following the schedule recommended in your device’s manual.
- Daily cleaning: Wipe down your mask cushion each morning and empty any remaining water from the humidifier chamber. Allow both to air-dry completely before reassembling.
- Weekly cleaning: Once a week, wash your mask, tubing, and humidifier chamber with warm, soapy water. Rinse everything thoroughly and let it air-dry away from direct sunlight or heat. You can also wipe down the machine’s exterior with a slightly damp cloth, but never submerge the machine or let water enter the air outlet.
Avoid using ozone or UV sanitizing devices, as the U.S. Food and Drug Administration (FDA) has raised concerns about their safety and effectiveness. Hand-washing with mild soap and water remains the safest and most reliable cleaning method.
How Do You Get a CPAP Machine?
Buying a CPAP machine involves a few important steps, starting with a sleep apnea diagnosis and ending with choosing the right device for your needs.
Do You Need a Prescription for a CPAP Machine?
In the United States, CPAP machines are classified as Class II medical devices, which means you need a valid prescription to buy one. A prescription ensures that your machine is set to the correct air pressure based on your sleep study results. If you haven’t been diagnosed yet, your doctor may recommend either an in-lab sleep study or a home sleep apnea test to confirm whether CPAP therapy is appropriate for you.
Where Can You Buy a CPAP Machine?
Once you have a prescription, you can purchase a CPAP machine from a variety of sources, including:
- Online retailers
- Durable medical equipment (DME) suppliers
- Some sleep clinics
Many people choose to shop online because it’s easier to compare models, read reviews, and select from a wider range of machines and accessories. Just make sure you purchase from an authorized seller to ensure your device is genuine and covered by a manufacturer warranty.
How Much Is a CPAP Machine?
The cost of a CPAP machine typically ranges from $500 to $1,000, depending on the model, features, and included accessories. More advanced devices—such as APAP or BiPAP machines—can cost significantly more. You'll also need to budget for ongoing replacement supplies, including filters, tubing, mask cushions, and humidifier chambers.
Does Insurance Cover a CPAP Machine?
Most private insurance plans, as well as Medicare and Medicaid, cover CPAP machines and related supplies when medically necessary. However, coverage varies widely by plan and may include additional requirements. Even with coverage, you may still be responsible for copays, deductibles, or part of the equipment cost. If you prefer to pay out of pocket, you can often purchase a CPAP machine directly and submit an itemized receipt for possible reimbursement through your insurer.
What Are the Benefits of Using a CPAP Machine?
Using a CPAP machine may provide several benefits if you have sleep apnea.
- Reduced or eliminated snoring: Snoring is a form of air flow resistance, and it may get better as a result of using CPAP.
- Restorative sleep: Since CPAP prevents mouth and throat tissues from blocking your airway, you're less likely to experience microarousals, or awakenings from deep stages to light stages of sleep. Fewer microarousals means you get more consistent, quality sleep.
- Reduced daytime sleepiness: Because you get more restorative sleep using CPAP, you’ll likely feel less sleepy and more energetic during the day.
- Improved daytime concentration: You may have improved concentration while doing daytime tasks when your sleep improves while using CPAP.
- Reduced blood pressure: CPAP can lower blood pressure and therefore may help slow the progression of serious health problems that are associated with high blood pressure.
- Diabetes prevention: Untreated OSA is associated with insulin resistance and type 2 diabetes. While data on this topic is limited, researchers suspect that CPAP may help regulate insulin and blood sugar levels and possibly prevent and treat type 2 diabetes.
What Are the Side Effects of CPAP Machines?
While CPAP machines can provide meaningful improvements, they can also have side effects. Fortunately, there are strategies you can take to minimize the effects of CPAP therapy and make treatment more manageable.
- Facial irritation: Sometimes the CPAP mask isn't the right fit, and if it’s too tight, it can put pressure on your skin and contribute to sores or ulcers. If this happens, tell your health care provider and start looking for a mask in a different size, a different model, or with a different cushioning material.
- Swallowing air: Swallowing air, also called aerophagia, can result in an upset stomach. Usually, switching to a nasal mask or nasal pillow will relieve this side effect. Alternatively, using an APAP machine or wearing a chin strap to keep your mouth closed while breathing through the nose can help prevent aerophagia.
- Claustrophobia: If you dislike confined spaces, then you may not like the contact a CPAP mask makes with your face. Try a different mask type, such as a nasal pillow, or resize your mask to make sure it fits properly.
- Air leaks: Sometimes if you breathe with your mouth but wear a nasal mask, the air that CPAP pumps into your nose can exit your mouth before it enters your airway. This is called a mouth leak. To resolve this, try wearing a chin strap to keep your mouth closed. You can also consider switching to a full-face mask.
- Nose or mouth dryness: Sometimes CPAP makes your upper airway feel chilly or dry. Adding a humidifier with a heated tube to your CPAP machine may help. If your nose feels stuffy, you could also try a decongestant or steroid nasal spray or switch to a full-face mask.
Are There Alternatives to CPAP Machines?
Although doctors typically recommend CPAP as a first line treatment, there are other treatment options for sleep apnea. Your doctor will help you choose the treatment option that works for you, your lifestyle, and preferences. The best choice is the one that improves your symptoms and that you feel comfortable using everyday.
Oral Appliances
Two oral appliances are gaining popularity among people with OSA.
- Mandibular advancement device (MAD): A MAD is a custom-fit, removable device that pushes your lower jaw forward, effectively opening your airway while you sleep. MADs have been shown to be as effective as CPAP at reducing sleep apnea symptoms, but CPAP does a better job of treating breathing disruptions and improving blood oxygen levels.
- Tongue-restraining device (TRD): A TRD is a plastic piece that uses suction to keep your tongue forward and away from your throat. More research is needed on this oral device, but it's an option for people who can’t use an MAD.
There are snoring mouth guards available in stores, but these aren't as comfortable or effective as MADs fitted by dentists. The mouth guards sold in stores may provide a false sense of security if they reduce your snoring, but don’t treat your sleep apnea. They may also adversely affect your jaw and the health of your teeth and gums.
Surgery
Surgery may be considered in a few situations for sleep apnea. Tissues of the nose, mouth, or throat that obstruct the airway in OSA and can be surgically corrected. Other types of surgeries implant a nerve stimulating device to help with breathing.
Although surgery can provide several benefits, such as improvements in snoring, daytime sleepiness, and quality of life, it typically doesn't completely eliminate OSA. So, after surgery, you may continue to use CPAP or an oral appliance.
When to See a Doctor
Consider contacting your doctor or a sleep specialist if you have signs of sleep apnea, which may include:
- Gasping or choking on air during sleep
- Loud, frequent snoring
- Feeling too sleepy during the day
- Not feeling well-rested after a full night of sleep
- Morning headaches
- Trouble paying attention or remembering things
Since some of these symptoms occur only during sleep, it’s important to take observations by your bed partner seriously.
When you meet with a doctor, they will likely ask you to participate in a sleep study, either in a lab or at home, to determine whether you have sleep apnea. If you're diagnosed with sleep apnea, then your doctor or health care provider may recommend trying CPAP therapy.
Frequently Asked Questions
A CPAP machine helps prevent breathing pauses from happening in the first place. By delivering a steady stream of pressurized air, CPAP keeps your airway open so it doesn’t collapse during sleep. If your airway begins to narrow, the pressure helps hold it open, reducing or eliminating apnea events and restoring normal airflow.
Modern CPAP machines are designed to be very quiet, typically producing around 25 to 30 decibels, which is similar to soft breathing or a whisper. Most people find the noise unobtrusive, and many users report that the steady sound becomes background noise that helps them fall asleep. If your machine seems unusually loud, it may be due to issues like mask leaks, worn-out filters, or improper setup.
Purified water is safer than tap water, but distilled water is the recommended option for CPAP humidifiers. Distilled water prevents mineral buildup, reduces the risk of bacterial contamination, and helps extend the life of the humidifier chamber. If purified water is all you have for a night or two, it’s generally acceptable temporarily, but you should switch back to distilled water as soon as possible.