At a Glance
Sleep apnea mouth guards (also called oral appliances) are dental devices worn during sleep that reposition the tongue or tongue and jaw to help keep the upper airway open. They're most often recommended for people with mild to moderate obstructive sleep apnea or for those who cannot tolerate CPAP therapy.
For people who struggle with CPAP therapy, there could be a simpler alternative. Wearing FDA-approved, custom-fitted mouth guards while sleeping is gaining popularity as a treatment option for obstructive sleep apnea (OSA). This type of mouth guard is typically customized by a qualified dentist, who works with your doctor to determine if oral appliance therapy is right for you.
Below, we'll cover different types of oral appliances for sleep apnea, how they work to improve OSA symptoms, and their strengths and weaknesses compared to other treatments.
Do Mouth Guards Help With Sleep Apnea?
Specially designed mouth guards can help treat mild to moderate OSA. These devices are removable oral appliances that keep your airway open while you sleep by adjusting the position of the jaw and tongue or just your tongue. This creates more space in the throat and can keep the upper airway from collapsing while a person sleeps, reducing snoring and interruptions in breathing associated with OSA.
Types of Sleep Apnea Mouth Guards
The two main types of sleep apnea mouth guards are mandibular advancement devices and tongue-retaining devices. Some newer devices are starting to become available, but because they're still being researched, less is known about their effectiveness in treating OSA.
Mandibular Advancement Devices (MADs)
A mandibular advancement device (MAD), also called a mandibular advancement splint or a mandibular repositioning device, is a plastic mouth guard that covers your upper and lower teeth. It moves your lower jaw forward by a few millimeters or more, which helps open the airway.
MADs can come as either one or two pieces. The one-piece option is more rigid and doesn’t allow the mouth to move as much as a two-piece, which has two separate components linked together.
A qualified dentist will take a digital scan or get an impression and bite registration of your teeth to ensure that the MAD is a good fit. Using this impression, a MAD can be customized by size, material, how much it covers the teeth, how much jaw movement it allows, and how far the lower jaw is advanced forward, among other characteristics.
Custom-Fit MADs vs. Premade MADs
Customized MADs are more effective, generally more comfortable, and more likely to fit well on the teeth than premade MADs available over the counter. Premade MADs, also known as “boil and bite” devices, are typically heated and molded by pressing them onto the teeth. These aren't as customizable or effective as those fitted by a dentist. Additionally, they're not FDA-cleared to treat sleep apnea, only snoring.
Another concern with over-the-counter MADs is that it’s possible to purchase these without a confirmed sleep apnea diagnosis and treatment supervision by a doctor. It’s important to work with a physician when pursuing MAD therapy, whether you’re interested in using an over-the-counter device or a customized mouth guard.
Tongue-Retaining Devices (TRDs)
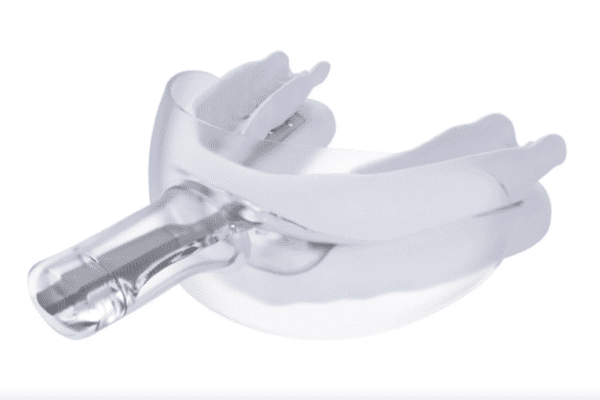
A tongue-retaining device (TRD) uses suction to keep the tongue in a forward position, preventing it from falling back into the airway. TRDs can be used by people who don't have enough teeth to keep a MAD in place or who can't use a MAD for other reasons.
TRDs haven't been as well-studied as MADs, so it’s less clear how effective they are at treating OSA. As a result, they're not prescribed or used as often.
A Simpler Way to Treat Sleep Apnea
Sleep Doctor’s oral appliances provide an alternative treatment designed for comfort, portability, and ease of use.

Mandibular Advancement Devices vs. Tongue-Retaining Devices
Though your doctor is ultimately the one who will decide what treatment option is best for you, here's a breakdown of the pros and cons of both types of mouth guards for sleep apnea.
| Type of Mouth Guard | Pros | Cons |
|---|---|---|
| Mandibular Advancement Devices | -Custom-fit options are available for better comfort and effectiveness -Often more discreet and compact than CPAP -May reduce both snoring and mild-to-moderate OSA symptoms -Allows for mouth breathing (unlike TRDs) | -Not suitable for people with TMJ issues or significant dental problems -Can cause jaw soreness or dental changes over time -May take time to adjust to wearing it nightly -Requires healthy teeth for a secure fit |
| Tongue-Retaining Devices | -Works even if you don’t have many teeth or wear dentures -No pressure on the jaw, making it a better choice for those with TMJ disorders -Simple design and usually less expensive than custom MADs -Often effective for people who can’t tolerate MADs | -Bulkier design may be less comfortable or harder to adjust to -Can cause tongue soreness or dry mouth -Less convenient for people who breathe through their mouths at night -May not stay in place as well during sleep |
Benefits of Sleep Apnea Mouth Guards
For people who dislike PAP therapy or have trouble using PAP therapy consistently, mouth guards may have several benefits. For example, mouth guards can be:
- Comfortable and non-invasive
- Effective for mild to moderate OSA
- Quiet
- Portable
- Easy to use and maintain
- Functional without a power supply
- Often covered by insurance
For these reasons, some people find mouth guards to be more manageable than CPAP and may use them with greater regularity.
Potential Risks of Sleep Apnea Mouth Guards
Wearing an oral appliance may cause symptoms to develop over time. Symptoms can include:
- Teeth discomfort
- Jaw joint pain
- Dry mouth
- Extra saliva production
- Gum irritation
- Teeth grinding
- Teeth shifting and loosening
- Bite changes due to the lower jaw shifting forward
These side effects are usually mild and temporary, often improving after a few weeks. It’s important to have follow-up visits with a dentist or health care provider to adjust the mouthpiece, make sure it fits properly and comfortably, and address any side effects that develop.
Effectiveness of Sleep Apnea Mouth Guards
Mandibular advancement devices are effective, but less so than CPAP, at reducing pauses in breathing and improving blood oxygen levels during sleep. However, research suggests that MADs perform similarly to CPAP when it comes to improving daytime sleepiness, reducing snoring, and lowering blood pressure. MADs may also reduce symptoms of depression and improve overall quality of life.
For some people, MADs are more comfortable than CPAP, making them more suitable for long-term use. MADs that are customized and fitted by dentists tend to be more comfortable and effective than premade MADs found in stores.
Although not as well studied, tongue-retaining devices may also reduce pauses in breathing, improve blood oxygen levels, and decrease daytime sleepiness.
Ultimately, OSA treatment can only be effective if a person uses it consistently. Some studies indicate that roughly half the people prescribed CPAP therapy don’t use it regularly or give it up completely. If these people find oral appliances more tolerable and are more willing to use them, they will be more likely to benefit from their treatment.
Sleep Apnea Mouth Guard vs. CPAP
Like CPAP machines, sleep apnea mouth guards are meant to be used only during sleep. But unlike CPAP machines, mouth guards don’t use forced air to keep the airway open. Instead, they rely on structural support and positioning, which is why many people find them more comfortable, especially if they have mild to moderate OSA or trouble tolerating CPAP.
CPAP is generally the most effective option, especially for moderate to severe sleep apnea. Mouth guards are often recommended for mild to moderate cases or for people who have trouble tolerating CPAP. They're smaller, quieter, and easier to travel with, but may not control symptoms as reliably as CPAP.
The best choice depends on the severity of your condition and what you can use consistently, and a healthcare provider can help guide that decision.
When Not to Use a Sleep Apnea Mouth Guard
While sleep apnea mouth guards are simple to use and often effective, they shouldn't be used in certain situations.
- Urgent need for therapy: People who have severe OSA or who feel very sleepy while driving may need to be treated immediately. Experts generally prefer CPAP for these cases because it takes less time to be effective, while finding the optimal fit for a mouth guard can take weeks or months.
- Low blood oxygen levels: If a person’s OSA causes blood oxygen levels to fall below 70% during sleep, an oral appliance may not be enough to significantly improve the problem.
- Certain dental conditions: MADs shouldn't be used by people who don’t have enough teeth to hold the device in place, who have disease or immobility of the jaw joint, significant periodontal disease, a gum infection, or who wear teeth realignment devices such as braces or retainers. Any pending dental work, including fillings or crowns, must be completed before the oral appliance is fitted.
- Central sleep apnea: Central sleep apnea (CSA) has a different cause than OSA. While in OSA the airway is blocked, in CSA, the brain fails to signal the body to breathe. Since a mouth guard only acts on the airway, it's not useful for people with CSA.
How to Get a Sleep Apnea Mouth Guard
Anyone can purchase a premade “boil and bite” mouth guard over the counter. But to obtain an effective and customized sleep apnea oral appliance, you must first receive a diagnosis of obstructive sleep apnea.
- Talk with your doctor about any symptoms you may have. Common OSA symptoms include gasping for air while asleep, loud snoring, morning headaches, daytime sleepiness, and trouble paying attention.
- If your symptoms suggest OSA, your doctor will likely order a sleep study. In a sleep study, your breathing patterns, heart rate, blood oxygen levels, and other metrics are measured while you sleep. These metrics are documented and interpreted by a sleep technologist, and the results are used to confirm an OSA diagnosis. For some people, an at-home sleep apnea test may be a viable option.
- After you are diagnosed with OSA, your doctor will discuss possible treatment options with you. CPAP is usually the treatment that health professionals recommend first. But if CPAP doesn't work for you, or if you're unable to tolerate CPAP and are unlikely to keep using it, your doctor may recommend an oral appliance as an alternative.
- The next step may be to see a qualified dentist who treats sleep apnea. Your dentist will examine your mouth health and your jaw mobility. If all looks healthy, your dentist will create a mold of your teeth to design your device and ensure it fits you well.
Adjusting Your Sleep Apnea Mouth Guard
After you get your MAD, your dentist will likely ask you to wear it every night. Over several weeks or months, your dentist will follow up with you and adjust how far the device moves your lower jaw forward. The goal of these adjustments is to open your airway as much as possible while maintaining your comfort while you sleep.
Monitoring Mouth Guard Effectiveness
Once your mouthpiece has been adjusted, your doctor and dentist may continue to follow up with you to learn whether your sleep apnea symptoms improve and whether new symptoms develop from wearing the mouth guard.
Even if your OSA symptoms have gotten better, the condition may still pose a threat. For this reason, your dentist will continually adjust your mouth guard. Your physician may recommend another sleep study after the mouth guard has been adjusted.
Frequently Asked Questions
Sleep apnea mouth guards are generally considered safe when properly fitted and prescribed by a qualified provider. Custom devices are designed to reposition the jaw or tongue to help keep the airway open. However, poorly fitting or over-the-counter devices may cause jaw discomfort, tooth movement, or irritation if used long-term. Regular follow-up with a dentist or sleep specialist helps ensure the device remains effective and comfortable.
The cost of a sleep apnea mouth guard can vary widely, depending on the type and how it’s obtained. Custom-fitted oral appliances prescribed by a dentist or sleep specialist typically cost between about $1,500 and $4,500, with many falling around $1,800 to $2,000 when including fittings and follow-up care. These higher-end devices are designed for comfort and effectiveness and are usually recommended for treating sleep apnea.
Lower-cost, over-the-counter mouth guards may be available for under $100, but they generally aren't as durable or effective for treating sleep apnea.
Many insurance plans, including some medical and dental policies, may cover sleep apnea mouth guards if they're medically necessary and prescribed by a qualified physician as part of a treatment plan. Coverage often depends on factors like the type of device, provider qualifications, and documentation of a sleep apnea diagnosis.
Because benefits vary widely, it’s best to check directly with your insurance provider to understand your coverage and any out-of-pocket costs.
Medicare may cover mouth guards for sleep apnea if they're prescribed by a doctor and provided by a qualified supplier as part of approved treatment. Coverage typically falls under durable medical equipment (DME) guidelines, and requirements such as a documented diagnosis and compliance may apply.
Because policies can vary, it’s important to check with Medicare or your provider for details about your specific plan.
A sleep apnea mouth guard should be cleaned daily to prevent bacteria buildup and maintain hygiene. Most devices can be rinsed with warm water and gently brushed with a soft toothbrush. It’s also important to let the device air dry completely and store it in a clean case. Some manufacturers recommend periodic deep cleaning with approved solutions. Always follow the specific care instructions for your device to help extend its lifespan and ensure safe use.
Medical Disclaimer: This content is for informational purposes and does not constitute medical advice. Please consult a health care provider prior to starting a new treatment or making changes to your treatment plan.
Still have questions?
Sleep apnea products can be confusing. If you need individualized assistance, post your question to the Sleep Doctor forum.