At a Glance
EPAP (expiratory positive airway pressure) therapy treats sleep apnea using small nasal devices that create resistance when you breathe out, helping keep the airway open during sleep. Unlike CPAP, EPAP does not require a machine, tubing, or continuous airflow, which may make it a simpler option for some people.
If traditional CPAP therapy feels uncomfortable or overwhelming, EPAP therapy may be another option worth exploring. EPAP, or expiratory positive airway pressure, uses resistance during exhalation to help keep the airway open without a machine, tubing, or continuous airflow.
For some people with mild to moderate obstructive sleep apnea (OSA), EPAP can provide a simpler and more portable alternative to CPAP. Below, we’ll explain how EPAP therapy works, who it’s best suited for, and how it compares to other sleep apnea treatments.
What Is EPAP?
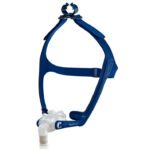
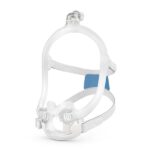
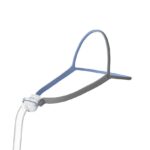
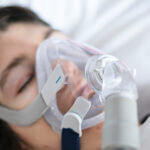
Nasal expiratory positive airway pressure (EPAP) is an emerging therapy for obstructive sleep apnea. An EPAP device consists of two valves that cover the nostrils as a person sleeps. When the sleeper exhales, these valves limit airflow and create sufficient pressure within the airway to prevent it from collapsing.
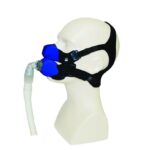
Unlike other PAP therapies, nasal EPAP doesn’t require a mask to keep the airway open during sleep. Instead, valves are secured in the nostrils or held in place with a strap that fits securely around the back of the head.
Although additional research is needed, several studies suggest that EPAP may be effective at improving symptoms for some people with OSA.
In one study, about half of the study participants had a 50% reduction in breathing disruptions after 3 months of EPAP use. The participants also found the EPAP device easy to wear all night. In another study, more than half of participants experienced a reduction in breathing interruptions and daytime sleepiness after a full year of EPAP use.
Think You May Have Sleep Apnea? Try an At-Home Test

our partner at sleepdoctor.com
10% off Home Sleep Tests
Buy Now“Truly grateful for this home sleep test. Fair pricing and improved my sleep!”
Dawn G. – Verified Tester
How Nasal EPAP Works
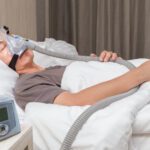
Nasal EPAP therapy uses small, valve-based devices that fit over the nostrils to help keep the airway open during sleep. When you inhale, air flows freely through the valves. When you exhale, the valves create gentle resistance, producing positive pressure in the airway. This back pressure helps prevent the soft tissues of the throat from collapsing, which can reduce snoring and breathing interruptions.
EPAP vs. CPAP
EPAP and CPAP are medical devices used to treat obstructive sleep apnea. Both treatments create positive pressure to prevent a person’s airway from collapsing during sleep. All devices designed to treat OSA, including CPAP and EPAP, require a prescription in the U.S.
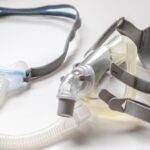
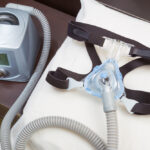
Continuous positive airway pressure keeps the airway open using a machine that pumps air through a hose and into a mask worn over the nose, mouth, or both. A CPAP machine delivers air at the same rate throughout the night to prevent the airway from collapsing. Some of the costs associated with CPAP are covered by medicare and many private health insurance providers.
In contrast, a nasal EPAP device doesn't require a mask, hose, or machine. Instead, an EPAP device is placed in the nostrils and keeps the airway open by limiting a sleeper’s exhalations. Unlike a CPAP device, EPAP devices do not require electricity or routine maintenance. EPAP devices may not be covered by health insurance providers.
| EPAP | CPAP | |
|---|---|---|
| How it works | Creates resistance during exhalation to generate airway pressure | Delivers continuous pressurized air to keep the airway open |
| Equipment required | Small nasal valves | Machine, tubing, and mask |
| Power source | None | Electricity required |
| Noise level | Silent | Low but audible |
| Portability | Highly portable; easy to travel with | Less portable; bulkier setup |
| Best for | Mild to moderate obstructive sleep apnea; CPAP-intolerant users | Mild to severe obstructive sleep apnea |
| Cost | About $200 | $500 to $2,000 |
| Insurance coverage | Limited or variable | Commonly covered by insurance |
How to Decide if EPAP Therapy Is Right for You
If you've been diagnosed with OSA, talk with your doctor or sleep specialist to determine the best sleep apnea treatment for you. Because nasal EPAP is an emerging technology, additional research is needed to determine the treatment’s effectiveness and appropriate candidates for this alternative to CPAP.
CPAP is a common method of providing positive airway pressure therapy, preferred by many doctors because of its familiarity and proven effectiveness. However, people who have difficulties tolerating CPAP devices may be appropriate candidates for EPAP.
Reasons why people may not tolerate CPAP include:
- Claustrophobia
- Discomfort from CPAP mask
- DIfficulties tolerating air pressure
- Congestion or nasal dryness
More research is needed to compare the effectiveness of EPAP and CPAP therapy. Although some studies have found that CPAP is better than EPAP at reducing the number of breathing interruptions per hour, other studies have found that CPAP is more effective or that both treatments are roughly equal in their ability to improve nighttime breathing.
EPAP therapy may be appropriate for people who cannot tolerate CPAP and who have mild to moderate OSA. Mild OSA is defined as 5 to 14 breathing interruptions per hour, while moderate OSA involves 15 to 29 interruptions each hour. EPAP may not be appropriate for people with severe OSA, who experience 30 or more breathing interruptions per hour.
Have a question for our experts? Submit it to the Sleep Doctor Forum.