At a Glance
If you snore, you only need a CPAP machine if you also have obstructive sleep apnea (OSA), which can only be diagnosed with a sleep study. If you don’t have OSA, lifestyle changes and other approaches may help you stop snoring.
Although it can disrupt a bed partner, snoring is often harmless. However, long-standing snoring, especially if it’s loud and frequent, can be a sign of sleep apnea. In adults, it’s estimated that 44% of males and 28% of females snore on a regular basis. That makes it all the more important to understand the difference between primary snoring and sleep apnea.
Below, we’ll explore the common causes of snoring, how to distinguish it from sleep apnea, when CPAP therapy is recommended, and the most effective approaches to reducing snoring.
Snoring? It Could be a Sign of Something More Serious

our partner at sleepdoctor.com
10% off Home Sleep Tests
Buy Now“Truly grateful for this home sleep test. Fair pricing and improved my sleep!”
Dawn G. – Verified Tester
What Causes Snoring?
Snoring is caused by the narrowing of the airway at the back of the throat, which causes the tissue in the walls of the throat to vibrate as you breathe. Often, the airway narrows simply because, during sleep, muscles relax and the tongue falls back in the mouth. However, blocked airflow can also be related to other health issues, including:
- Sleep-related breathing disorders, like obstructive sleep apnea (OSA)
- Nasal congestion
- Swelling of the tonsils, adenoids, soft palate, or other sedatives
- Excess body weight or obesity
- Use of alcohol, sleeping pills, or other substances that relax muscles
- Some facial features, like a large tongue or deviated septum
Does Snoring Mean Sleep Apnea?
Snoring is not the same thing as sleep apnea. Snoring is a common symptom of obstructive sleep apnea, but that doesn’t mean all snoring is linked to sleep apnea. Many people who snore do not have sleep apnea. In fact, there are some people who have OSA and don’t snore.
Almost everyone snores on occasion, and even habitual snoring can have many different causes that aren’t sleep apnea. As a result, you can’t determine whether someone has sleep apnea based on snoring alone. Your doctor will consider snoring in the context of any other symptoms and physical findings to decide whether a sleep study is warranted to diagnose OSA.
Is It Snoring or Sleep Apnea?
Primary snoring, which refers to habitual snoring that is not caused by airway collapse or sleep apnea, is different from OSA-related snoring. However, the only way to know for sure which type is through a sleep study. There are a few distinctions, though, that you can share with your doctor.
In terms of sound, OSA-related snoring tends to be louder, more frequent, and consistent over time. In addition, people with OSA are much more likely to experience snoring that’s occasionally punctuated by gasping, snorting, or choking.
Beyond the sound itself, OSA-related snoring is different in how it affects the body. For people with OSA, narrowing of the airway also causes repeated decreases in blood oxygen levels. Low oxygen levels provoke extremely brief awakenings to restore breathing, and these recurring episodes disrupt sleep quality.
Primary snoring doesn’t have these effects on oxygen levels or sleep quality. As a result, typical snoring doesn’t pose the same health risks as sleep apnea. Untreated OSA causes excessive daytime sleepiness and can increase the risk of serious complications, including:
- Car accidents from drowsy driving
- High blood pressure, heart attack, stroke, and other cardiovascular problems
- Type 2 diabetes
- Liver disease
- Impaired concentration, memory, and decision-making
Over time, it’s possible for regular snoring to progress to obstructive sleep apnea. Studies have found that gaining weight is a significant risk factor for primary snoring to develop into OSA.
Can CPAP Stop Snoring?
Using a continuous positive airway pressure (CPAP) machine is an effective way to stop snoring. That said, a CPAP for snoring is usually only prescribed when the snoring is related to obstructive sleep apnea.
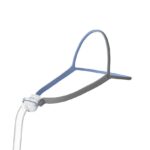
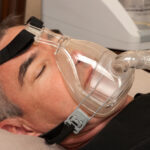
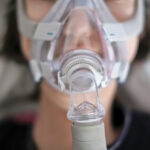
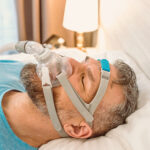
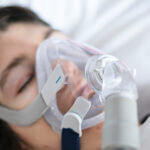
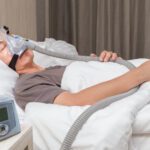
For CPAP therapy, you wear a mask connected to the CPAP machine by a long tube. The machine pumps pressurized air through the tube and mask, creating an incoming stream of air that holds your airway open. In this way, a CPAP machine can prevent the airway narrowing that causes snoring.
When Is CPAP Recommended?
CPAP therapy is prescribed for people diagnosed with moderate or severe obstructive sleep apnea. It isn’t usually prescribed for people who snore but don’t have sleep apnea.
CPAP therapy is the most common treatment for OSA. It’s often the first treatment prescribed because it can effectively treat most cases of OSA, preventing snoring and other breathing disruptions while improving sleep quality.
FDA rules require a prescription to get a CPAP machine. To get a prescription for OSA, you must first be diagnosed with the condition, which requires sleep testing.
One way of testing for OSA is by doing an overnight test in a specialized sleep lab. During this type of sleep study, sensors monitor your breathing, heart rate, and brain waves, allowing technicians to identify OSA and other sleep disorders.
Another option is at-home testing for OSA. An at-home sleep test measures your heart rate, blood oxygen levels, and other data that can be used to diagnose moderate and severe OSA.
In addition to determining whether a person has OSA, these tests also calculate how many breathing-related sleep disruptions occur per hour, also called the apnea-hypopnea index (AHI). This data is essential for determining the severity of OSA.
Why Isn’t CPAP Recommended for Primary Snoring?
There are two main reasons why doctors don’t usually recommend or prescribe CPAP therapy for primary snoring alone without a suspicion of possible OSA.
- Lack of insurance coverage: Because snoring in itself doesn’t pose any well-established health risks, insurance companies generally won’t cover the cost of a CPAP machine unless a person also has a diagnosis of OSA.
- Challenges of CPAP therapy: Using a CPAP machine can be inconvenient and cause side effects like discomfort and dry mouth. Even for people with OSA, sticking with CPAP therapy can be a challenge. This makes it even less likely that someone with simple snoring will actually use a CPAP device every night.
What Are Other Ways to Stop Snoring?
A number of approaches can help reduce or stop snoring. These include lifestyle changes, new health habits, and other ways of keeping the airway from narrowing during sleep.
Side Sleeping
If you normally sleep on your back, switching to your side is one change that can significantly reduce snoring. When you sleep on your back, gravity pulls your tongue and other tissues in the neck toward the airway, increasing the chances of snoring. Side sleeping helps avoid this, but you may find it challenging to sleep on your side if your natural position is on your back.
Different products are available to help you stay on your side, including specialty pillows and sleeping position alarms. You can even try sewing a tennis ball into the back of your pajamas to discourage back sleeping.
Avoiding Alcohol and Tobacco
Research suggests that avoiding alcohol and tobacco at night can reduce snoring. Alcohol, in particular, decreases muscle tone, making the tissue in your throat more likely to fall into a position that blocks your airway.
Weight Management
Having obesity is a risk factor for snoring, so maintaining a healthy weight may decrease how much you snore. Keeping a stable, healthy weight may also help prevent you from developing obstructive sleep apnea in the future.
Treating Nasal Congestion
Having a stuffy nose makes it more likely that you’ll snore, so treating nasal congestion can be a useful step toward stopping snoring, assuming that's the underlying cause. When your nose is congested, you must generate more force through your airway when you breathe, and this added force can contribute to snoring. You can talk with your doctor about the cause of your congestion and the best way to treat it.
Oral Appliances
Sometimes called mouthguards or mouthpieces, oral appliances are devices that hold your jaw and tongue in place so that they don’t narrow your airway. Studies have found that oral appliances are effective at stopping snoring, and people often find them more comfortable to use than a CPAP machine.
Different types of oral appliances are available, and the best results frequently come from getting a custom-fitted device from a dentist.
Nasal Strips
Nasal strips go over the middle of your nose and are held in place by an adhesive. As you breathe, they help hold your nostrils open. Although evidence about their effectiveness is mixed, they may be recommended as a low-risk option if snoring is the result of poor airflow through the nose.
Anti-Snoring Exercises
Anti-snoring exercises, formally known as myofunctional therapy, are designed to build tone in the muscles of the tongue, mouth, and throat. Several studies have found that regularly doing these exercises can decrease the frequency and loudness of snoring.
Surgery
Surgery may be a treatment option for snoring when anatomical issues contribute to airway obstruction. For example, surgery may be able to remove excess tissue in the soft palate that relaxes and blocks the airway during sleep. Because there can be complications and short-lived results, doctors generally recommend multiple other conservative options to treat snoring before trying surgery.
Have a question for our experts? Submit it to the Sleep Doctor Forum.