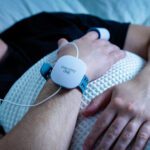
The SleepView At-Home is a sleep apnea test made by CleveMed, a medical device company, that can be completed in the comfort of your own home. The small, lightweight device measures eight data points through three wearable components, allowing medical professionals to determine whether you have sleep apnea. The machine can complete a multi-night sleep study and reports the data in a secure patient web portal.
At-home tests are a great option for individuals who suspect they might have sleep apnea and prefer to complete a test at home. We’ll discuss the features of the SleepView At-Home, how the machine compares to in-lab sleep studies, and how to use the device so you can determine if it’s the right test for your needs.
At a Glance
The SleepView has multiple sensors that measure eight different data points to help doctors diagnose sleep apnea. The setup process is straightforward, and the device supplies feedback to let users know if the device is tracking data.
Ideal For
- People looking for an at-home sleep apnea test that collects high-quality data
- Those wishing to sleep in their own bed for the duration of the test
- Individuals needing a device that has an auxiliary port for optional testing components
Who Should Keep Looking
- Individuals who need an in-lab sleep test
- People suspected to have central sleep apnea
- Those not wanting to set up a sleep apnea testing device
-
Price
$3,200
-
Dimensions
3″ x 2.6″ x 0.7″
-
Test Location
Chest, nostrils, and finger
-
Weight
2 oz.
Use this SleepApnea.org link for the most current discount on the SleepView
Shop NowOverview of the CleveMed SleepView
The SleepView is designed to detect OSA symptoms with multiple sensors that measure eight different data points, helping medical professionals make an accurate diagnosis. The device comes with easy-to-follow instructions, and a setup video is available on the company’s website. Sensor lights make it easy for users to see if the device is connected and collects enough data. While most users will only need to test for one night, the device can also be used for a multi-night sleep study.
What's Included
The SleepView At-Home device includes an effort belt, pulse oximeter, nasal cannula, and instructions. Your doctor may also supply you with a questionnaire and additional auxiliary device, such as an IDcheck, second effort belt, or thermistor.
- Monitor
- Effort belt
- Pulse oximeter
- Nasal cannula
- User guide
- AAA battery
- Carrying case
- Optional auxiliary devices (IDcheck, second effort belt, or thermistor)
Notable Features
- Ultracompact: The device weighs 2 ounces and measures 3 inches wide, 2.6 inches tall, and .7 inches thick. The small, lightweight design allows users to sleep with minimal disturbance.
- Sensor check: The device verifies all sensors are properly connected before you begin the study.
- Smart check: After completing the test, the device indicates whether it recorded quality data via sensor lights, letting the user know if they need to repeat the study.
- Multiple sensors: The device monitors eight data points. These metrics include heart rate, blood oxygen level, respiratory airflow, respiratory effort belt, snoring, body position, integrated actigraphy, and an auxiliary port.
- Web portal: The secure patient web portal provides access to sleep test data, scoring, and interpretation of the results.
- Auxiliary port optional devices: The auxiliary port can be used with one of three devices depending on each sleeper’s needs.
- IDcheck helps verify the sleeper’s identity with adhesive stickers worn under clothing during the day and connected via a cable to the device at night. Some insurance companies require this for reimbursement.
- A second effort belt allows doctors to get a more accurate reading of a user’s breathing patterns.
- A thermistor assists with measuring airflow and is held in place by the nasal cannula.
Technical Specifications
The SleepView has several features designed to make testing easy and comfortable for users. The device’s ultra-compact design allows for users to sleep with minimal disturbance. Other features such as sensor check and smart check make it easy for users to tell if the study was successful.
Don't Just Test Your Sleep. Understand It.
With Sleep Doctor’s home sleep study, you’ll get a personalized medical report and expert consultation, so you can take the next step with confidence.

How the SleepView Works
The SleepView collects high-quality sleep data by measuring eight different data points. The device helps medical professionals determine a user’s AHI through several metrics.
What It Measures
- Heart rate: The pulse oximeter measures your heart rate. A person’s heart rate will fluctuate before, during, and after experiencing apneas. This helps doctors determine if changes in heart rate accompany any changes in breathing patterns.
- Pulse oximetry: The pulse oximeter also measures the amount of oxygen in your blood. People with OSA experience lower blood oxygen levels after apnea events, which can also worsen sleep apnea symptoms.
- Respiratory airflow (compatible with CPAP): The nasal cannula measures a sleeper’s airflow during exhalation and inhalation to help doctors see irregular breathing patterns and determine a user’s AHI. This component is compatible with continuous positive airway pressure (CPAP) machines, which allows healthcare professionals to track the airflow of individuals during therapy.
- Respiratory inductance plethysmography (RIP): Respiratory inductance plethysmography (RIP) is a non-invasive measurement of a person’s chest movement during breathing, also known as respiratory effort. The effort belt measures this, helping doctors track your breathing quality.
- Amount of snoring: Loud, frequent snoring is one of the most common symptoms of OSA. The nasal cannula measures the number of snoring episodes.
- Body positioning: The device tracks when users sleep on their side, back, stomach, or in an upright position. This helps your healthcare team see if your sleep apnea symptoms change when you switch sleeping positions.
- Auxiliary: The auxiliary port has three additional sensor options, including IDcheck, a second effort belt, and a thermistor.
- Integrated actigraphy: This metric tracks body movement to determine how often a user wakes up throughout the night.
Types of Sleep Apnea This Device Detects
The SleepView is designed to determine if a person has OSA. If your doctor suspects you may have central sleep apnea (CSA) they will consider an in-person sleep study or look for an at-home test that can detect symptoms of CSA. While it’s possible to have both OSA and CSA simultaneously, CSA is only present in 1% of the population. Talk with your doctor about testing options if you suspect you might have CSA.
Medical professionals diagnose OSA by measuring your breathing patterns in a sleep study. Doctors monitor the average amount of times you experience apneas and hypopneas during one hour of sleep to determine your apnea-hypopnea index (AHI). Apnea refers to pauses in breathing, and hypopnea refers to shallow breathing. Your AHI score can also determine your sleep apnea severity.
| AHI Score | Sleep Apnea Severity |
|---|---|
| 5-15 | Mild OSA |
| 15-30 | Moderate OSA |
| 30+ | Severe OSA |
How to Use the SleepView
Your healthcare team will provide you with specific instructions on how to use the SleepView. CleveMed recommends wearing the device over a lightweight shirt. Sleepers should wear the device for at least six hours to ensure enough data is recorded.
- Connect the belt: First, connect the monitor to the belt. You should hear two clicks when they connect. Wrap the strap around your chest and adjust the Velcro tabs to achieve a snug but comfortable fit. Those with breasts can place the belt above or below them. The device should rest in the center of your chest.
- Attach the nasal cannula: Insert the nasal cannula prongs into your nostrils. Wrap the tubing around your ears and move the slide toward your chin. Place a piece of medical tape over the tubing on each cheek to ensure it stays in place. Connect the end of the cannula to the device by turning it clockwise to lock it in place.
- Connect the pulse oximeter: Plug the pulse oximeter into the monitor before placing your index finger in the sensor. The finger icon should face up. Secure the wire on the back of your hand with a small piece of medical tape. Remove any nail polish or acrylic nails beforehand to prevent inaccurate readings.
- Attach the auxiliary device: The device includes an additional auxiliary port for an IDcheck, second effort belt, or thermistor. The instructions can guide you on how to attach each device to the monitor. If you don’t have an auxiliary device, the auxiliary sensor light will remain off.
- Start the test: To begin the test, press the “on” button for three seconds until the power light turns green. An amber light signifies a sensor needs to be adjusted. If a light is red, it means the wire is not properly connected to the device. Sensor lights stay on for 90 seconds after the device is turned on, and the power light will remain on for the duration of the test.
- Go to sleep: Once the device is ready, you can go to sleep. CleveMed recommends spending part of the night sleeping on your back. If you wake up during the night, keep the sensors and device on, even if you go to the bathroom. If any sensors become disconnected, simply reattach them.
- After waking up: When you wake up in the morning, press the “off” button for three seconds. The device recorded successfully if the lights turn green and move in a clockwise pattern. If the lights appear red in a counterclockwise direction, review the instruction sheet for tips on how to set up another test.
- Complete paperwork: Answer the questionnaire and complete any other necessary paperwork before returning the device to your healthcare provider.
Sleep Data Results and Diagnosis
Once you return the device to your healthcare provider, it can take up to two weeks to receive results. However, most people have access to the data in the patient portal within one week. Your doctor will schedule a time to discuss your results and treatment options, if necessary.
SleepView vs. In-Lab Sleep Studies
In-lab sleep studies are the standard for diagnosing sleep apnea. However, at-home sleep apnea tests can be a good option for individuals who have OSA symptoms and don’t have any other health conditions. Those who have trouble sleeping when outside their home, want a cost-effective option, and don’t want to wait to schedule an appointment with a sleep lab should consider an at-home test. If your doctor suspects that you have CSA or other sleep disorders, you’ll need to consider other testing options.
| SleepView | In-Lab Sleep Study | |
|---|---|---|
| Benefits |
|
|
| Limitations |
|
|
Customer Reviews
Individuals who used the SleepView report being pleased with the overall process and enjoyed the option to complete a sleep study in the comfort of their home. Most people found it easy to follow the instructions and set up the device. Others noted how quickly they received their results after returning the device.
Trial, Warranty, and Shipping Policies
| Availability | The device is not available for individuals to purchase, as doctors rent it out to multiple people. Since the SleepView is only available for medical professionals to purchase, availability will vary depending on your individual healthcare provider. |
| Shipping | Shipping and turnaround time depend on your healthcare provider. The device comes with setup instructions and your doctor will instruct you on what to do with the device after completing the test. |
| Warranty | Most people will only use the SleepView for one night and then return it to their healthcare team. Medical professionals can purchase the device through CleveMed. Each purchase includes a one-year warranty. |
Frequently Asked Questions
Obstructive sleep apnea (OSA) occurs when a person’s airway becomes narrowed or blocked during sleep, resulting in periodic pauses in breathing. Several factors can increase a person’s likelihood of having OSA, such as obesity, frequent nasal congestion, alcohol use, and enlarged tonsils.
Many different symptoms are associated with OSA, and each person experiences different ones. However, there are some symptoms that are more commonly experienced. Individuals with OSA often feel sleepy or tired throughout the day, regardless of how much sleep they got the night before. They may also be forgetful, irritable, or impatient. Some people may fall asleep during activities like reading, watching TV, working, or driving.
Sometimes, those with sleep apnea don’t know they have it until a family member mentions they have a pattern of heavy snoring sometimes followed by gasping or snorting. Individuals who have untreated OSA may also show signs of depression, high blood pressure, and morning headaches.
The SleepView does not replace a CPAP titration study. The SleepView is only designed to detect OSA, and individuals may still need to complete a titration study after diagnosis. A CPAP titration study determines the correct air pressure settings for your CPAP machine.
Medical Disclaimer: This content is for informational purposes and does not constitute medical advice. Please consult a health care provider prior to starting a new treatment or making changes to your treatment plan.
Still have questions?
Sleep apnea products can be confusing. If you need individualized assistance, post your question to the Sleep Doctor forum.